Cancer genetics
Is this cancer a hereditary cancer?
About 5% to 10% of breast cancer cases are thought to be hereditary, meaning that they result directly from gene changes (mutations) passed on from a parent. The most common cause of hereditary breast cancer is an inherited mutation in the BRCA1 or BRCA2 gene.
Hereditary genes
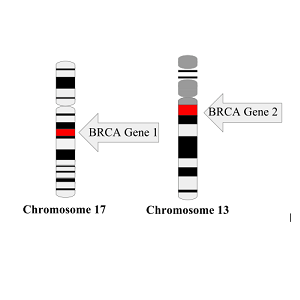
The most common cause of hereditary breast cancer is an inherited mutation in the BRCA1 or BRCA2 gene. In normal cells, these genes help make proteins that repair damaged DNA. Mutated versions of these genes can lead to abnormal cell growth, which can lead to cancer.
- On average, a woman with a BRCA1 or BRCA2 gene mutation has up to a 7 in 10 chance of getting breast cancer by age 80.
- Women with one of these mutations are more likely to be diagnosed with breast cancer at a younger age, as well as to have cancer in both breasts.
- Women with one of these gene changes also have a higher risk of developing ovarian cancer and some other cancers.
- Men who inherit one of these gene changes also have a higher risk of breast and some other cancers.
- In the United States, BRCA mutations are more common in Jewish people of Ashkenazi (Eastern Europe) origin than in other racial and ethnic groups, but anyone can have them.
[Note: BRCA, which is short for BReast CAncer, is usually pronounced either by saying “brah-kuh” or by saying “B” “R” “C” “A”.]
Source: “Inheriting certain gene changes” (American Cancer Society, 2021)
BRCA Genes and Breast Cancer
Without treatment, a woman who is BRCA1 or BRCA2 mutation carrier is seven times more likely to develop breast cancer and 30 more times likely to develop ovarian cancer before the age of 70.
A 3-minute video from the CDC.
Understanding BRCA Mutations and Risk
Everyone has the BRCA genes. Their job is to repair errors that occur in your cell’s DNA. If one or both genes you inherited have a mutation, they might let some errors through.
A 4-minute video from the Dr. Susan Love Foundation.
Dispelling myths of BRCA gene mutations
BRCA mutations have been linked to breast, ovarian, pancreatic and prostate cancers, all of which aside from ovarian cancer, can affect men.
A 4-minute video from AstraZeneca.
Black & BRCA is a collaboration between the Basser Center for BRCA and its team of patient advocates, researchers and healthcare professionals to bring tailored resources and support to the Black community. The Basser Center is part of the University of Pennsylvania Health System, a major multi-hospital health system headquartered in Philadelphia, Pennsylvania.
“At a time when Black men and women are more likely than the general population to be diagnosed with cancer at later stages when it is less treatable, Black & BRCA seeks to empower individuals to understand their family health history and take action to prevent cancer from one generation to the next.”
Educational Resources
"I had known a long time that the mutation was a possibility"

“I learned in 2007 that my mom carried a BRCA2 mutation after she was diagnosed with breast cancer for a second time. Children of mutation carriers have a fifty percent chance of carrying the mutation as well. By the time I underwent genetic testing in 2014, I had known for a long time that carrying the mutation was a possibility,” says lawyer and cancer activist Erika Stallings.
“When I got my genetic testing results, my oncologist recommended that I have a preventative mastectomy as soon as possible given my family history. I was 29 when I received my test results and my mother had breast cancer for the first time when she was 28 years old.”
“I would advise all Black women to take the time to learn their family health history. If you have a family history of cancer, you likely need to start screenings such as mammograms and MRIs before the age of 40 and you may need to consider genetic testing. I always tell people that the patient/provider relationship is a partnership. If your doctor is unresponsive when you bring up risk for breast cancer, find a provider that will take your concerns seriously.”
Source: Black & BRCA interview with Erika Stallings on the Black Girl Affirmed website
Read more at Erika Stallings’ website.
BRCA gene mutations in men
 Men with a mutation in the BRCA2 gene also have an increased risk of breast cancer, with a lifetime risk of about 6 in 100. BRCA1 mutations can cause breast cancer in men, too, but the risk is lower, about 1 in 100. BRCA mutations also increase the risk of prostate and pancreatic cancers in men.
Men with a mutation in the BRCA2 gene also have an increased risk of breast cancer, with a lifetime risk of about 6 in 100. BRCA1 mutations can cause breast cancer in men, too, but the risk is lower, about 1 in 100. BRCA mutations also increase the risk of prostate and pancreatic cancers in men.
Although mutations in these genes most often are found in members of families with many cases of breast and/or ovarian cancer, they have also been found in men with breast cancer who did not have a strong family history.
Mutations in CHEK2, PTEN and PALB2 genes might also be responsible for some breast cancers in men.
Source: Risk Factors for Breast Cancer in Men (American Cancer Society, 2018)
For more information about signs, symptoms, diagnosis and treatment of breast cancer in men, see “Breast Cancer in Men” on the American Cancer Society website.

While cancer risks in male BRCA mutation carriers are not as dramatically elevated as those of female BRCA mutation carriers, cancer risk management and early detection are vital.
It is important for both men and women to remember that a family history of breast, ovarian, prostate or pancreatic cancers on their father’s side of the family may indicate a hereditary gene mutation.
Many people mistakenly believe a family history of breast or ovarian cancer only matters on their mother’s side of the family. Men can inherit a BRCA gene mutation from their mother or father and can pass on their BRCA gene mutation to their male and female children.
Medical management for men with BRCA1/2 mutations changes at age 35–40. Ages at which screenings begin are dependent on family history and should be discussed with a physician.
For more information about screening and genetic testing, see “BRCA1 and BRCA2 in Men” on the Basser Center for BRCA website.
Beyoncé's father is a BRCA carrier and cancer survivor
Mathew Knowles, 67, a music industry executive and father of singer Beyoncé, noticed blood spots on the new white T-shirts his wife Gena bought him in 2019. “I said, oh, maybe it’s something to do with these shirts,” he remembered. But when Gena found blood on the sheets on his side of the bed, an alarm bell went off.
Early in his business career, Knowles worked for Xerox selling breast cancer diagnostic imaging equipment to hospitals and health facilities. A breast discharge, he had learned, was one of the signs of male breast cancer.
“So I immediately called my referring physician, said I need to get a mammogram. We got one immediately like the next day and then we got a biopsy.” Diagnosis: breast cancer. A few days later, Knowles had a unilateral mastectomy.
Genetic testing revealed he carried a BRCA2 gene mutation. His family history suddenly made sense. His maternal aunt and her two daughters had died of breast cancer and four of this father’s brothers died from prostate cancer. BRCA mutations increase the risk of both cancers.
Knowles is now cancer-free. Beyoncé and her sister Solange have tested negative for the mutated BRCA2 gene, according to reports in the media.
5 minute video from American Association for Cancer Research
Other genes involved in breast cancer
- ATM
- BARD1
- CDH1
- CHEK2
- NF1
- PALB2
- PTEN
- RAD51C
- RAD51D
- STK11
- TP53
- CHEK2
- PALB2
Disparities in breast cancer genetics?
African American and White Women share same genes that increase the risk of breast cancer
 The same genes that increase the risk of breast cancer in U.S. White women also greatly increase breast cancer risk among African American women. Previous studies of women of African ancestry were too small to assess genes other than BRCA1 and BRCA2.
The same genes that increase the risk of breast cancer in U.S. White women also greatly increase breast cancer risk among African American women. Previous studies of women of African ancestry were too small to assess genes other than BRCA1 and BRCA2.
“This means that the multi-gene panels that are currently available to test women diagnosed with breast cancer or women at high risk due to their family history will be useful for African American women,” explains Julie Palmer, ScD, (left) of the Boston University School of Medicine.
Researchers in 2020 sequenced the germline (inherited) DNA from 5,054 African American women with breast cancer and 4,993 age-matched African American women without cancer for mutations in 23 genes linked to a predisposition for cancer. They then estimated the risks of developing breast cancer associated with having a mutation in any of the genes.
- Source: “African American and White Women Share Genes that Increase Breast Cancer Risk” on the Boston University School of Medicine website
- See the full text of the scientific paper “Contribution of Germline Predisposition Gene Mutations to Breast Cancer Risk in African American Women” by Julie R Palmer et al.
Rates of genetic mutations similar between Black and White women diagnosed with breast cancer
 In a 2021 study of 3,946 Black women diagnosed with breast cancer and 25,287 White women also diagnosed with the disease, the rates of genetic mutations in genes linked to breast cancer were similar. Among the Black women, 5.65% had a mutation in one of the 12 genes, compared with 5.06% of the White women, a difference that is not statistically different.
In a 2021 study of 3,946 Black women diagnosed with breast cancer and 25,287 White women also diagnosed with the disease, the rates of genetic mutations in genes linked to breast cancer were similar. Among the Black women, 5.65% had a mutation in one of the 12 genes, compared with 5.06% of the White women, a difference that is not statistically different.
The researchers, led by Susan Domchek, MD, (right) of the University of Pennsylvania, concluded that all efforts should be made to ensure equal access to genetic testing to minimize disparities in care and outcomes in women diagnosed with breast cancer.
- Source: “Do Black Women Diagnosed With Breast Cancer Have Higher Rates of Genetic Mutations Than White Women?” by Jamie DePolo on the breastcancer.org website
- See the full text of the scientific paper “Comparison of the Prevalence of Pathogenic Variants in Cancer Susceptibility Genes in Black Women and Non-Hispanic White Women With Breast Cancer in the United States” by Susan M. Domchek et al.
Recent news about disparities in genetic mutations
Breast cancer genetic testing
Get Genetic Counseling Before Testing

The Centers for Disease Control and Prevention (CDC) says it’s important to get genetic counseling before genetic testing for hereditary breast and ovarian cancer in order to determine whether you and your family are likely enough to have a mutation that it is worth getting tested. Usually, genetic testing is recommended if you have:
- A strong family health history of breast and ovarian cancer
- A moderate family health history of breast and ovarian cancer and are of Ashkenazi Jewish or Eastern European ancestry
- A personal history of breast cancer and meet certain criteria (related to age of diagnosis, type of cancer, presence of certain other cancers or cancer in both breasts, ancestry, and family health history)
- A personal history of ovarian, fallopian tube, or primary peritoneal cancer
- A known BRCA1, BRCA2, or other inherited mutation in your family
Carletta (above) tested negative for BRCA mutations after being diagnosed with breast cancer.
Source: “Genetic Testing for Hereditary Breast and Ovarian Cancer” (CDC)
How is genetic testing done?

Genetic testing is typically done only if you and your health care team feel that it’s the best thing for you and your family. The first step is to collect information about your personal and family medical history. A genetic counselor or other trained professional will go over this information to help determine:
- Your risk of developing cancer,
- If genetic testing might be helpful for you, and
- If so, what specific gene changes should be tested for
Even if the counselor recommends you be tested, you still have the right to refuse it.
Genetic tests for cancer are typically done on a sample of blood, saliva, or cheek cells from swabbing the inside of your mouth). Once the results are ready (often 2-3 weeks later), your genetic counselor will share the results with you.
For more reasons to seek genetic counseling, see “Genetic testing for people who have been diagnosed with breast cancer” (FORCE: Facing Hereditary Cancer Empowered)
Susan G. Komen says its “My Family Health Portrait” is an internet-based tool that’s easy to access on the web and simple to fill out and should only take about 15 to 20 minutes to build a basic family health history. It assembles your information and makes a “pedigree” family tree that you can download and share with family members or send to your health care practitioner. It is private–it does not keep your information.

Don’t rely on direct-to-consumer genetic testing to determine your BRCA status. More than 1,000 variants of the BRCA genes are known to increase the risk of cancer. 23andMe genetic testing , the only FDA-authorized, Direct-To-Consumer BRCA Test, detects only the three variants most common in people of Ashkenazi Jewish descent. These variants are rarely found in people of other ethnicities, the company cautions.
If you had genetic testing before 2014 that was negative for breast cancer mutations, you might want to consider getting an updated gene test. Genetic tests before 2014 did not include testing for important BRCA mutations, the PALB2 gene and other mutations.
Genetic testing after a breast cancer diagnosis
Genetic testing may be recommended after a diagnosis of breast cancer to look for gene mutations that have been inherited. Some breast cancer treatments are given only to people who have certain inherited gene mutations.
Knowing about inherited mutations and the risk of cancer can also be important information for other family members.

Testing for gene mutations within the tumor itself may also be done. For some people, this can help guide treatment.
More at: Genetic Testing After a Breast Cancer Diagnosis (Susan G. Komen)
Paying for genetic testing
Insurance coverage for genetic counseling and testing
 Most health plans cover genetic counseling and testing for inherited gene mutations linked to cancer in people who meet the national guidelines. The cost of testing and your out-of-pocket charges may vary based on several factors. People who are denied coverage for genetic testing can file an appeal (FORCE has sample appeal letters). About half of appeals are approved.
Most health plans cover genetic counseling and testing for inherited gene mutations linked to cancer in people who meet the national guidelines. The cost of testing and your out-of-pocket charges may vary based on several factors. People who are denied coverage for genetic testing can file an appeal (FORCE has sample appeal letters). About half of appeals are approved.
Medicare and Medicaid
Genetic counseling and testing is typically covered by Medicare for people already diagnosed with cancer who are in treatment or for whom test results may affect their care. Most state Medicaid programs cover genetic testing for BRCA and Lynch Syndrome mutations for people who meet requirements, which vary by state. You can read more about Medicare and Medicaid coverage of genetic testing here.
Financial assistance or low cost genetic testing
JScreen is a national program based out of Emory University in Atlanta that provides discounted at-home genetic counseling and testing with financial assistance available. Many laboratories offer low-cost genetic testing or financial assistance programs. Programs vary, so if you are not eligible for assistance through one lab, consider contacting other labs to see if you qualify. For more information, see “Paying for Care” on the FORCE website.
Disparities in breast cancer genetic testing?
Racial Disparities Persist in Genetic Testing

Carlette Burton knew she had a family history of cancer, but she never looked into her genetic risk for BRCA-related cancer until she found a concerning lump in her breast during a self check. After her diagnosis, she had genetic testing done and found out that she has a BRCA mutation.
Burton’s mother also had been diagnosed with breast cancer in her 30s. Her grandmother had had breast cancer, too. She is one of five sisters, “but I don’t ever recall a doctor saying we should get tested.”
Read more at “Racial disparities still persist in genetic testing for BRCA-related breast cancer” by Tracey Romero on the Philly Voice website (April 6, 2021)
Black women less likely to undergo genetic counseling and testing
About five percent of both Black and white women have a genetic mutation that increases their risk of breast cancer, according to a new study of nearly 30,000 patients.
However, compared to White women, Black women are much less likely to undergo genetic counseling and testing, largely due to differences in physician recommendations or access to care.
“Our efforts should focus on ensuring equal access to testing to minimize disparities in care and outcomes,” said researcher Susan Domchek of Penn Medicine at the University of Pennsylvania (June 11, 2021)
Read more at “Black and White Women Have Same Mutations Linked to Breast Cancer Risk” on the Penn Medicine website (June 11 , 2021)



